 
Require minimal movement of the affected painful hip.For trauma: “Cross Table Lateral” or “Horizontal Beam Lateral” has these views.There are multiple ways to perform the “lateral view”.A standard “hip series” consists of the AP view of the pelvis and a lateral view of the affected extremity.2 visits: Bring patient back for repeat filmsĪn approach to the traumatic adult hip x-ray.2 occasions: Always compare with old x-rays if available.2 sides: If unsure regarding a potential pathologic finding, compare to another side.2 joints: Image above and below the injury.2 abnormalities: If you see one abnormality, look for another.MRI hip protocols can be done in as little as 5-15 minutes.īefore we begin: Make sure to employ the rule of 2’s Consider MRI for patients with significant hip pain and negative x-rays. 2% of occult hip fractures will be missed by CT.Compared with CT, pelvic radiographs have a sensitivity of 64% to 78% for the identification of pelvic fractures in blunt trauma. 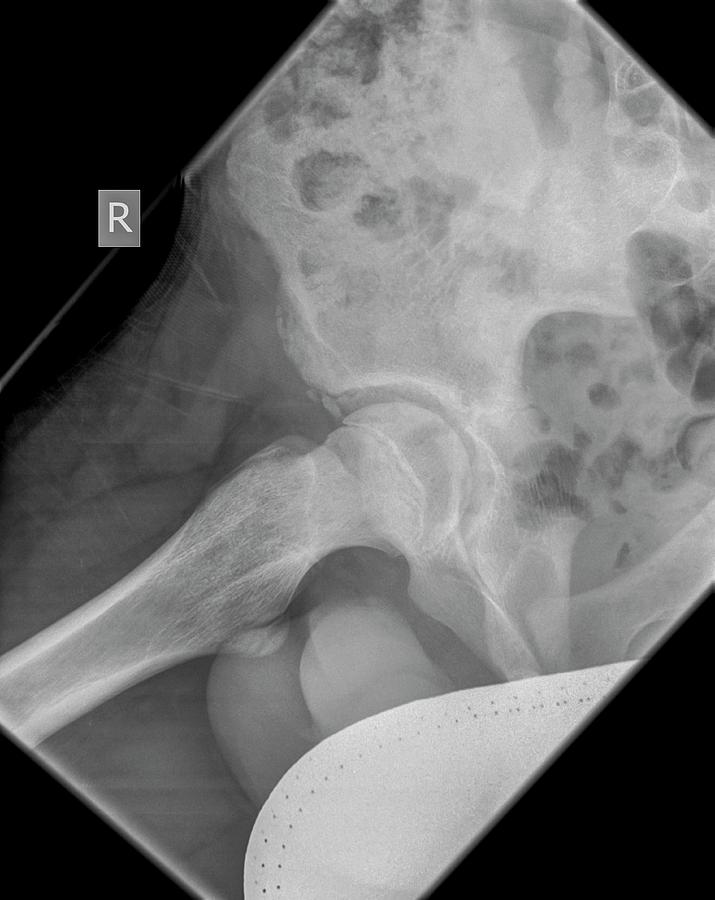
Hip fractures have a very high one-year mortality.Hip and thigh pain are common complaints in the ED.Why the hip matters and the radiology rule of 2’s The Hip Identify clinical scenarios in which an additional view might improve pathology diagnosis.Interpret traumatic hip x-rays using a standard approach.When applicable, it will provide pertinent measurements specific to management, and offer a framework for when to get an additional view, if appropriate. PubMed PMID: 25205017.This is EMRad, a series aimed at providing “just in time” approaches to commonly ordered radiology studies in the emergency department. Systemic biochemical markers of joint metabolism and inflammation in relation to radiographic parameters and pain of the knee: data from CHECK, a cohort of early-osteoarthritis subjects. , 2 Van Spil WE, Nair SC, Kinds MB, Emans PJ, Hilberdink WK, Welsing PM, Lafeber FP. Predictive validity of biochemical biomarkers in knee osteoarthritis: data from the FNIH OA Biomarkers Consortium. In the future, doctors may be able to test blood or joint fluid for biomarkers that predict or identify the osteoarthritis.ġ Kraus VB, Collins JE, Hargrove D, Losina E, Nevitt M, Katz JN, Wang SX, Sandell LJ, Hoffmann SC, Hunter DJ OA Biomarkers Consortium. See What Is Arthrocentesis (Joint Aspiration)? Lab tests may require a blood draw or an aspiration of the hip joint, during which fluid is taken from the hip. A physician may use ultrasound along with an injection of local anesthetic (intraarticular injection) to try to identify the exact source of pain.Ī doctor may order lab tests to diagnose or rule out other potential problems, such as infection or types of inflammatory arthritis, which can also cause hip pain. Ultrasound can also be used to identify changes to the delicate membrane that surrounds the joint (synovial lining) or an abnormal increase in joint fluid (synovial fluid). Ultrasound can be useful for evaluating the soft tissue structures that surround the hip joint, such as tendons, bursae, muscles, and the edge of the labrum. MRIs tend to be more time-consuming and more expensive than x-rays. A doctor may order an MRI if the x-rays are inconclusive or he or she suspects something other than osteoarthritis, such as damage to the hip’s labrum. Magnetic Resonance Imaging (MRI) can provide images of the hip’s soft tissues (such as the hip labrum, articular cartilage, and tendons) as well as bone. Therefore, x-rays are just one tool to be used with the patient interview and physical exam. Conversely, x-rays may show only mild osteoarthritis but the patient reports significant pain. X-rays may show significant signs of hip osteoarthritis and yet the patient may not be in pain. These growths can create additional friction that can lead to pain. Bone spurs are a normal sign of aging-almost everyone over age 50 has some-but they may proliferate as bones try to compensate for cartilage loss. Small bumps on the bones, called bone spurs or osteophytes.No space or an abnormally small space indicates a loss of cartilage. How much space there is between the femur and the acetabulum of the pelvic bone (the hip’s ball and socket). 
Hip osteoarthritis can be confirmed with x-rays. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
